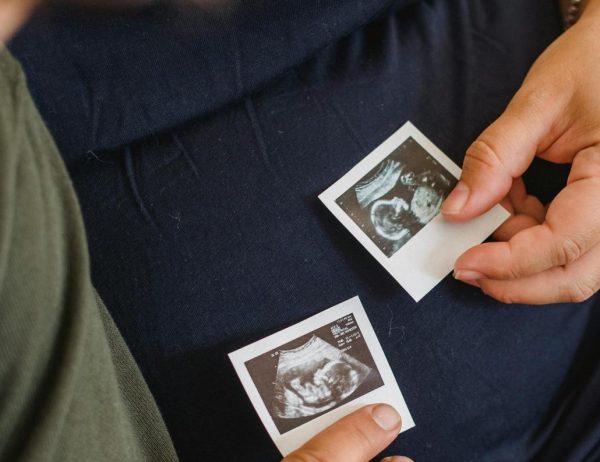
High-tech mannequins give real-world experience to paramedicine students
Lindenwood’s paramedicine students are using high tech mannequins to practice medical procedures.
Photo by Mitchell Kraus
March 2, 2018
Video by Michelle Sproat
MATT HAMPTON | Reporter
During lab in the basement of Hyland Arena, first responders assessed the patient’s symptoms. They checked the pulse, the blood pressure, then jotted down notes on their gloves and hooked up an IV.
But the patient in this emergency wasn’t real; he was a lifesized mannequin. And the first responders were students in Lindenwood’s paramedicine program, one of the university’s newest majors.
The simulations involve four high-tech mannequins that students began using this semester.
An iPad controls the mannequins’ reactions, things like dilating a pupil or turning lips blue. The simulations also include defibrillators, electrocardiogram machines and other emergency equipment.
“We can change their EKG if they have some lung issues like in a traumatic situation,” said Darrell DeMartino, one of the assistant professors in the program.
When treated correctly, a mannequin’s EKG and lung sounds will return to normal, he said.
The mannequins can cry and salivate, and their right shin allows for intraosseous infusion, a process by which a drug is injected directly into the bone marrow, said adjunct instructor Ryan Pattiz.
The paramedicine program was created last year, after an Emergency Medical Technician course was offered during summer semester. The labs constitute half of the paramedicine degree.
Training center coordinator Janet Schulte said getting access to real patients, like those giving birth, has become more difficult.
“They say ‘If you’re just there to watch, I don’t want you there,’” Schulte said.
So in addition to the new mannequins, Lindenwood will be using the SmartMom birthing simulator this fall, she said. The device can even simulate delivery complications, such as hemorrhaging.
Not all of the features of the new mannequins are being used in class yet, but they are gradually introducing more complex situations as the students learn more advanced skills. Next semester will include scenarios related to trauma, children, births and chest injuries.
DeMartino said that though the mannequins take some getting used to, students generally like them because they are so realistic. DeMartino, who has worked as a paramedic and a nurse practitioner, said technology allows for more complex and immersive simulations.

Photo by Mitchell Kraus
“About eight years ago, the ones that breathe used to have a compressor that had to be in another room,” he said. “Now we’ve moved to wireless, and we can actually put the compressor inside the leg for example, so we can get the breathing motion to occur without all of the technology.”
According to Cynthia Schroeder, the dean of the school of health sciences, Lindenwood’s paramedicine bachelor’s program provides graduates with better opportunities because it is more intensive and includes courses such as pharmacology and pathophysiology.
“Most of what you might see out in the field right now are paramedics who have been trained in a certificate type of a program,” she said. “In our program they are getting more of a holistic experience.”
Student Bradley Gaylord enrolled in the program after a stint in the Marine Corps. He said the paramedicine program provides a more detailed understanding of the science behind treatment, and the mannequins play a big role.
“When we first started the program … we were using each other, just kind of imagining things were happening,” he said. “When we learned something as simple as vital signs, with seven healthy students in an EMT class, you’re not going to get any abnormal vital signs.”
Program director Nick Miller said the degree requires at least four full-time semesters and about 700 to 800 hours of clinicals, exceeding the state requirement of 500 hours.
Paramedicine courses are organized into eight-week blocks focused on a single subject, with lecture on Tuesday and Thursday and lab on Wednesday and Friday. In addition to class four days a week from 8 a.m. to 1 p.m., paramedicine students also work a 12-hour clinical shift at least once a week.
Students start doing clinicals at several St. Louis-area hospitals their first semester and transition into doing them in an ambulance by the end of the program.
Gaylord said as the students get to know people at the hospitals, they are getting to do more skills during the clinicals.
“They can be fast-paced, they can be busy, but they’re fun experiences,” he said.
In their final semester, paramedicine students do a field internship in which they have much of the responsibility of a working paramedic.
Gaylord said he began taking EMT classes as a step toward becoming a firefighter, but he is now considering a career as a paramedic.
“Once I started learning more about the body and more about the medicine and stuff and how everything works, I really actually fell in love with it,” he said